Έκφραση πολυμεράσης στο μυελοδυσπλαστικό σύνδρομο
Abstract
Introduction
Poly [ADP-ribose] polymerase 1 (PARP-1) has a central role in the repair of single-stranded DNA breaks, thus protecting the cell from genomic instability. Overexpression of PARP1 may lead a cell to apoptotic or necrotic death, defining the cell’s fate. Genetic defects are important in the pathogenesis of myelodysplastic syndromes (MDS) and the role of PARP1 in the apoptotic pathways seems to be promising, since new agents targeting PARP1 are available. PARP1 expression has never been studied in MDS.
Uridine-Cytidine Kinase (UCK) catalyzes the phosphorylation of uridine and cytidine as well as the pharmacological activation of several cytotoxic pyrimidine ribonucleoside analogues. The UCK family consists of two members, UCK1 and UCK2, both expressed in several tumor cell types. UCK2 in particular has been found to be expressed in pancreatic tumors, neuroblastoma and other malignant cells, but not in normal tissues, although it is normally expressed in human placenta. The selective expression of UCK2 in certain tumor cells enables selective malignant cell targeting with UCK2-dependent pyrimidine analogues, while sparing normal tissues.
Aim
Our aim was to detect PARP1, UCK1 and UCK2 mRNA in bone marrow samples of patients with MDS and investigate its correlations to the hematologic and prognostic characteristics of the patients.
Patients and Methods
Bone marrow samples were collected from patients with MDS. Quantification of PARP1 mRNA was performed by a SYBR-green based Real-Time PCR, and the results were expressed in correlation to those of the housekeeping gene of beta actin. Quantification of UCK1 and UCK2 was performed by a Real-Time PCR using specific oligonucleotides and TaqMan probes (Applied Biosystems, CA, USA) and all experiments were normalized to the housekeeping gene of glyceraldehyde-2-phosphate dehydrogenase (GAPDH). All reactions were performed on BIORADCFX96 (BIORAD Laboratories, CA, USA).
PARP1 protein was also detected by western-blot using both simple films and the Azure c300 Chemiluminescent Western Blot Imaging System (Azure Biosystems, CA, USA).
Results
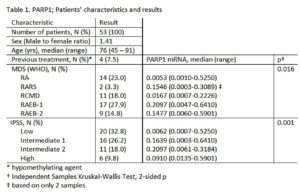
Fifty seven (57) patients with MDS were included in the study. The basic demographic and hematologic characteristics of the patients are shown in Table 1. The vast majority of the patients (92.9%) were treatment naïve. PARP1 mRNA levels were measured in 53 patients, while UCK1 and UCK2 mRNA levels were measured in all patients.
The median PARP1 mRNA levels were 0.0259 (range 0.0003 – 0.6410) and showed a statistically significant correlation to the type of MDS (according to the WHO classification) (p=0.016) and to the IPSS score (p=0.001) (detailed results in Table). The lowest levels were observed in patients with RA (0.0053 vs 0.1477 for non-RA patients, p= 0.016), as well as in patients with low and intermediate 1 IPSS score (0.0107 vs 0.1831, p=0.01) that had almost 20 times lower PARP1 mRNA levels than patients with intermediate 2 and high risk MDS.
The protein could only be detected in samples tested with the Azure c300 Chemiluminescent Western Blot Imaging System. The median value of PARP1 expression was 0.298 (0 – 1.625) and no correlations with the WHO classification or the IPSS were detected. To our knowledge, PARP1 detection by western blotting has never been performed in the past in MDS.
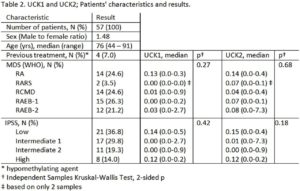
Although both UCK1 and UCK2 were detected in the majority of the patients (40/57, 70.2% for UCK1 and 15/57, 73.7% for UCK2), no correlation was found between their levels and the type of MDS or the prognostic factors according to the IPSS or WPSS. The median levels were for UCK1 0.0202 (0 – 2.7431) and for UCK2 0.0169 (0 – 7.270). Detailed results are presented in Table 2.
Conclusions
The correlation of higher levels of PARP1 mRNA with higher risk MDS has never been reported in the past. This correlation, if confirmed by larger studies, may render PARP1 a prognostic factor for patients with MDS. Moreover, this result can lay the basis for the design of clinical trials evaluating the use of PARP1 inhibitors in patients with higher risk MDS. Although we didn’t detect any correlation of UCK1 and UCK2 with the prognostic characteristics of MDS, their mere detection in clinical samples of patients with MDS is significant, since these molecules are not detected in every malignancy, but just in a subset of malignant diseases. This finding could be of value since targeted therapies are already available.
Article Information
- Published online December 1, 2016.
- Panagiotis Theodorou Diamantopoulos, 1Laikon General Hospital, First Department of Internal Medicine, National and Kapodistrian University of Athens, Athens, Greece
- Panagiotis Zervakis, 1Laikon General Hospital, First Department of Internal Medicine, National and Kapodistrian University of Athens, Athens, Greece
- Maria Sofotasiou, 1Laikon General Hospital, First Department of Internal Medicine, National and Kapodistrian University of Athens, Athens, Greece
- Konstantinos Zervakis, 2National and Kapodistrian University of Athens, Laikon Hospital, 1st Department of Internal Medicine, Athens, Greece
- Argiris Symeonidis [MD PhD], 3Hematology, University of Patras Medical School, Patras, Greece
- Kodandreopoulou Elina, 4National and Kapodistrian University of Athens, Laikon General Hospital, 1st Department of Internal Medicine, Athens, Greece
- Galanopoulos Athanassios, 5Department of Clinical Hematology, “G. Gennimatas” District General Hospital, Athens, Greece
- Pappa Vassiliki [MD PhD], 6Haematology Division, 2nd Department of Internal Medicine, Attikon General Hospital, National and Kapodistrian University of Athens, Athens, Greece
- Kotsianidis Ioannis, 7Department of Hematology, University Hospital of Alexandroupolis, Alexandroupolis, Greece
- Christopoulou Georgia, 8Department of Internal Medicine, University Hospital of Patras, Patras, Greece
- Papadopoulou Vasiliki, 9First Department of Internal Medicine, National and Kapodistrian University of Athens, Laikon General Hospital, Athens, Greece
- Mantzourani Marina [MD PhD], 9First Department of Internal Medicine, National and Kapodistrian University of Athens, Laikon General Hospital, Athens, Greece
- Nora-Athina Viniou [MD PhD], 101st Department of Internal Medicine, Hematology Unit, National Kapodistrian University of Athens, Laikon General Hospital, Athens, Greece